Cervical Health Awareness Month
January is Cervical Health Awareness Month, sponsored by the National Cervical Cancer Coalition (NCCC) it is a time to bring awareness to the issue of Cervical Health. Each year approximately
14,000 women in the United States will be diagnosed with Cervical Cancer. Cervical Cancer is preventable with appropriate vaccination and screening and that’s something worth celebrating.What is Cervical Cancer?
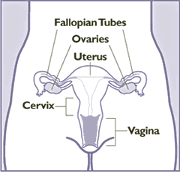
The US Department of Health and Human Services defines Cervical Cancer as “cancer of the cervix, which is the low, narrow part of the uterus that connects the uterus to the vagina. Abnormal cells in the cervix can turn into cancer if doctors don’t find and treat them.”
Almost all cases of cervical cancer are caused by certain types of HPV (human papillomavirus). Some types of HPV cause genital warts, and others cause cancer. HPV is the most common infection spread through sex.
The majority of HPV infections go away on their own. In some case an HPV infection may last for a long time, these can cause cancer.
Prevention and Detection
The CDC recommends receiving the HPV Vaccination starting with preteens aged 11 to 12 years old. HPV vaccination also is recommended for everyone through age 26 years, if they are not vaccinated already. HPV vaccination is not recommended for everyone older than age 26 years. The HPV vaccine works best when given before any exposure to HPV. Persons age 27 to 45 that haven’t received the HPV vaccine, should consult with their doctor to determine if the HPV Vaccine is right for them.
When it comes to Detection the CDC recommends getting screened or tested for cervical cancer. This means getting tested before any symptoms have appeared. Screening tests for cervical cancer include:
- Pap tests, also called Pap smears
- HPV (human papillomavirus) tests
These tests can help in the detection of cervical cancer. They can also identify cervical cells that are infected with HPV or other abnormal cells before they turn into cancer. Most cases of cervical cancer can be prevented by regular screenings — and the right follow-up treatment when needed. Women should get their first Pap test at age 21. If these test results are normal, doctors advise waiting three years before the next test.
Women aged 30 to 65 have a range of options available when it comes to screening and testing.
- Getting a Pap test only. If your test result is normal, you can wait three years for your next test.
- Getting an HPV test only. If your test result is normal, you can wait five years for your next test.
- Getting both an HPV and Pap test together. If your test results are normal, you can wait five years for your next tests.
Women age 66 or older, should consult with their doctor to determine if they need to continue getting screened for cervical cancer.
What happens during cervical cancer screening tests?
Cervical cancer screening tests usually happen as part of a pelvic exam. During this exam, you lie on your back on an exam table, bend your knees, and put your feet into stirrups.
While you lie on the exam table, the doctor or nurse will put a medical tool (called a speculum) into your vagina and open it to see your cervix. The doctor or nurse will use a special brush to collect some cells from your cervix. Then the doctor or nurse will send these cells to a lab, where an expert will check for abnormal cells or for the types of HPV that can cause cervical cancer.
These tests take about 5 minutes. It may feel uncomfortable, but it usually doesn’t hurt. If you’re not comfortable being alone with the doctor or nurse during the exam, ask to have another health professional from the practice (like another nurse) in the room, too.
Screening Test Results
Results from both the HPV and PAP tests will help in determining if the HPV virus is present or if there is cervical cell changes or abnormalities.
HPV Results
Results of HPV testing will come back as either Positive or Negative. HPV test results usually come back from the lab in about 1–3 weeks.
A Positive HPV test result will typically indicate a High-risk HPV was found. The health care provider will recommend follow-up steps to take based on the specific test results.
A negative HPV test result will typically indicate that High-risk HPV was not found. However, the health care provider may advise for a more frequent interval for the next examination if there have been abnormal results in the past.
Sometimes, after several negative HPV tests, a patient may experience a positive HPV test result. This may be a result of having a new sexual partner, this is most likely a new infection. In some instances, a prior HPV infection can become active again after many years resulting in a new positive result. There is no way to tell whether a newly positive HPV test result is a sign of a new infection or a reactivation of an old infection. Researchers don’t know whether a reactivated HPV infection has the same risk of causing cervical cell changes or cervical cancer as a new HPV infection.
PAP Test Results
Pap test results are used to determine whether cervical cells are normal or abnormal. A Pap test may also be identified as unsatisfactory.
Normal Pap test results: No abnormal cervical cells were found.
Unsatisfactory Pap test results: The lab sample may not have had enough cells, or the cells may have been clumped together or hidden by blood or mucus.
Abnormal Pap test results: An abnormal test result may also be called a positive test result. Some of the cells of the cervix look different from the normal cells. An abnormal test result does not mean you have cancer. Your health care provider will recommend monitoring, more testing, or treatment.
Abnormal Pap test results include
Atypical squamous cells of undetermined significance (ASC-US): This is the most common abnormal Pap test finding. It means that some cells don’t look completely normal, but it’s not clear if the changes are caused by HPV infection. Other things can cause cells to look abnormal, including irritation, some infections (such as a yeast infection), growths (such as polyps in the uterus), and changes in hormones that occur during pregnancy or menopause. Although these things may make cervical cells look abnormal, they are not related to cancer. Your health care provider will usually do an HPV test to see if the changes may be caused by an HPV infection. If the HPV test is negative, estrogen cream may be prescribed to see if the cell changes are caused by low hormone levels. If the HPV test is positive, you may need additional follow-up tests.
Atypical glandular cells (AGC): Some glandular cells were found that do not look normal. This can be a sign of a more serious problem up inside the uterus, your healthcare provider will likely ask you to come back for a colposcopy.
Low-grade squamous intraepithelial lesions (LSIL): There are low-grade changes that are usually caused by an HPV infection. Your health care provider will likely ask you to come back for additional testing to make sure that there are not more serious (high-grade) changes.
Atypical squamous cells, cannot exclude high-grade squamous intraepithelial lesion (ASC-H): Some abnormal squamous cells were found that may be a high-grade squamous intraepithelial lesion (HSIL), although it’s not certain. Your healthcare provider will likely ask you to come back for a colposcopy.
High-grade squamous intraepithelial lesions (HSIL): There are moderately or severely abnormal cervical cells that could become cancer in the future if not treated. Your healthcare provider will likely ask you to come back for a colposcopy.
Adenocarcinoma in situ (AIS): An advanced lesion (area of abnormal growth) was found in the glandular tissue of the cervix. AIS lesions may be referred to as precancer and may become cancer (cervical adenocarcinoma) if not treated. Your healthcare provider will likely ask you to come back for a colposcopy.
Cervical cancer cells (squamous cell carcinoma or adenocarcinoma): Cancer cells were found; this finding is very rare for people who have been screened at regular intervals. If a biopsy shows that cervical cancer is present, your doctor will order certain tests to find out if cancer cells have spread within the cervix or to other parts of the body. See the Cervical Cancer Diagnosis page for information about tests that may be used to diagnose and stage cervical cancer.
Follow up after an abnormal PAP or a Positive HPV Test
- Return for a repeat HPV test or HPV/Pap cotest in 1 or 3 years
- have a colposcopy and biopsy
- receive treatment;
Colposcopy
During a colposcopy, a doctor inserts a speculum to gently open the vagina and see the cervix. A vinegar solution is applied to the cervix to help show abnormal areas. The Healthcare Provider then places an instrument called a colposcope close to the vagina. It has a bright light and a magnifying lens and allows the doctor to look closely at the vagina and cervix for abnormal areas.
A colposcopy usually includes a biopsy, so that the cells or tissues can be checked under a microscope for signs of disease, including cervical cancer.
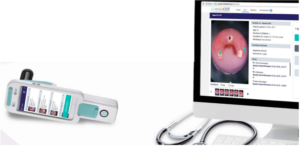
How USC Supports Cervical Health
Ultrasound Solutions is proud to continue in providing awareness and the diagnostic tools for healthcare providers in supporting women’s health exams. Ultrasound Solutions is a distributor of the MobileODT EVA Colposcope a hand held device for easy examination and smooth workflow. The EVA Colposcope is a light and portable, complete digital solution for magnified cervical visualization, documentation and teleconsultation.